Arthritis
Arthritis is a chronic condition that causes pain, swelling, and inflammation in the joints. Common joints impacted by arthritis include knees, hips, hands, feet, spine, and shoulders. There are more than 100 types of arthritis and related conditions. While there is no cure, there are ways for you to manage arthritis pain.
To serve you better, please set your location for information on services available in your area.
What are the symptoms of arthritis?
The symptoms of arthritis may vary depending on your type and the severity of the disease.
- Most forms of arthritis will cause pain, stiffness, and swelling.
- Your pain may be constant or intermittent.
- Some people experience a dull ache, while others have sharp, searing pain.
- People with autoimmune arthritis may notice warmth or redness around the joint.
- Bumps and other disfigurements are possible as well.
What is arthritis?
Arthritis is a condition that happens when the smooth covering on the ends of bones wears away. This covering is a rubbery tissue called cartilage, which helps joints move easily and without pain. When cartilage wears down, the bones can rub against each other, causing damage over time.
Hip with arthritis vs. healthy hip
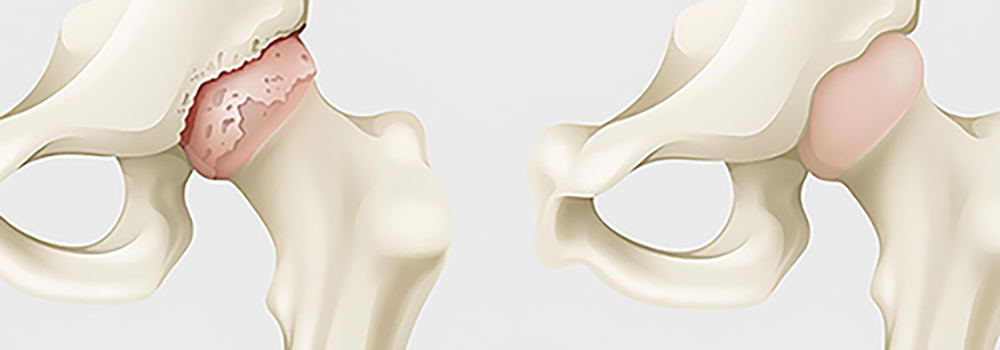
This graphic shows a damaged hip bone due to the loss of the smooth covering (cartilage) on the ball of the hip. It also shows a normal hip bone with the cartilage in place.
What are the different types of arthritis?
Osteoarthritis, the most common form of arthritis, is often linked to aging. However, other types can affect people of all ages. You might have it as the result of an injury or an autoimmune response. The four most diagnosed forms of arthritis are:
Osteoarthritis
Osteoarthritis is a degenerative disease caused by the thinning of the cartilage in your joints.
- As the most common form of arthritis, osteoarthritis impacts over 32.5 million U.S. adults.2
- Your knee, hip, spine, and hand are most likely to be affected.
- As cartilage breaks down everyday activities can cause pain, stiffness, and reduced movement.
Psoriatic arthritis
Psoriatic arthritis is an inflammatory disease associated with skin plaques over the knees and elbows. It often arises in middle age in people with psoriasis.
- Up to 30% of people with psoriasis also suffer from psoriatic arthritis.3
- It may affect one or more of your joints and can cause severe damage, if not treated.
Rheumatoid arthritis (RA)
Rheumatoid arthritis is a serious inflammatory disease of the joints. RA occurs when your autoimmune system attacks its own tissues.
- It affects the lining of your joints (synovium) and can damage the tissues covering the end of bones.
- Over time the inflammation destroys the cartilage and bone, leading to deformities.
- RA can also cause fever and fatigue, and at times affect organs such as the heart, eyes, and skin.
- A rheumatologist provider can develop a treatment plan for RA and other autoimmune conditions.
Gout
Gout is a buildup of crystals in the joints that leads to sudden, severe pain.
- It is more common in males than females.
- It typically impacts smaller joints such as the big toe.
Who is at risk for arthritis?
The primary causes of arthritis can vary by type, and all of us have some level of risk. Disease, genetics, injury, infection, and aging can all play a role. Some of the more common risk factors include:
- Age — As we age, our joints sustain damage from overuse, which causes osteoarthritis.
- Sex — In general, women are more likely than men to develop most forms of arthritis.
- Injury — A serious joint injury, at any age, can cause post-traumatic osteoarthritis.
- This is more likely to occur in lower extremities. Symptoms may go away within a few months, or it may turn into a chronic condition.
- Autoimmune disorders — RA and similar types of arthritis are triggered when the body attacks its own cells.
- Genetics and lifestyle — If you have a family history of arthritis, or you are overweight, diabetic, or smoke, you have a higher risk of the disease.
How is arthritis diagnosed?
Diagnosis begins with a medical history and physical exam. Your doctor will check the movement of your joints and look for signs of swelling, redness, or warmth. Your doctor may order lab tests to analyze your blood, and possibly fluid from your joint. X-rays are the initial test of choice to diagnose arthritis. Occasionally other imaging studies such as a CT scan or MRI are needed.

How is arthritis treated?
If arthritis pain impacts your everyday life, talk to your doctor about your options. Your doctor may prescribe one or more treatment options to help reduce your pain and symptoms. Treatment options may include:
Lifestyle changes
- The best defense against arthritis is regular exercise, maintaining a healthy weight, and having a balanced diet.
Medications
- NSAIDs (nonsteroidal anti-inflammatory drugs) and Tylenol help with arthritis pain relief and swelling.
- Topical NSAIDS are available as gels, liquids, creams, and patches.
- DMARDs (Disease-modifying antirheumatic drugs) used for RA slow down or stop inflammation, keeping arthritis from progressing.
- Other medications may be used for gout, psoriatic arthritis, and other forms of arthritis due to a medical condition. Talk to your doctor about what might be right for you.
Injections
- Cortisone injections can help reduce pain and swelling.
- Hyaluronic acid injections may also be used to reduce pain and swelling
Physical therapy
Physical therapy is a valuable tool for arthritis management. It can help with your pain, improve your function, and restore motion.
Surgical procedures:
If your arthritis pain is not helped by other treatments, your doctor may recommend a surgical option. Surgery cannot always cure or reverse arthritis, but it can remove damaged areas and improve quality of life. Treatment options might include:
Arthroscopy is a minimally invasive procedure to fix tissue tears and repair the damage of the smooth covering on the bone (cartilage). It is best suited for younger patients to reduce pain and restore movement.
It uses pins, plates, and other hardware to connect bones in the ankle, wrist, finger, or spine. The bones will grow together over time to lock the joint in place.
Partial and total joint replacement focuses on replacing the worn out joint surfaces. It has a proven record for safety and success in reducing pain and improving range of motion.
Common questions about arthritis:
There is no evidence that habitual cracking of knuckles (or any bone or joint) causes arthritis. However, one study found that knuckle crackers are more likely to have hand swelling and lower grip strength.4
Osteoarthritis is an age-related disorder with roughly 54% of adults 75 and older receiving a diagnosis.2
Osteoarthritis is a degenerative condition. It can be hard to know if worsening problems are a temporary flare or a sign of progression. Since it is not an autoimmune disease triggered by internal processes, flares are more likely to be caused by external issues. Overexertion, trauma, infection, weight gain, or even cold weather can be culprits.
If you've tried less invasive treatments and your quality of life is still suffering, you may want to consider surgery. Our orthopedic team will assess your pain and level of function to determine the best option for you.
Foods that contribute to inflammation may trigger pain and other symptoms. You may benefit from an anti-inflammatory diet that restricts certain types of foods. Try limiting red/processed meat, refined carbohydrates, heavily sweetened and fried foods, and alcohol.
Incorporate anti-inflammatory foods into your meals. Examples of foods include: fish, berries, leafy greens, nuts, seeds, olive oil, broccoli, brussels sprouts, cauliflower, oranges.
Both heat and cold can be beneficial, depending on the individual and the cause of pain.
- Cold therapy may reduce inflammation, swelling, and pain.
- Heat can relieve stiffness.
Alternating heat and cold can be helpful. Experimenting with both therapies is a good way to determine what works best for you.
- Arthritis basics. (2024, March 22). Arthritis. https://www.cdc.gov/arthritis/basics/index.html
- Osteoarthritis Action Alliance. (2025, March 18). OA Prevalence and burden - Osteoarthritis Action Alliance. https://oaaction.unc.edu/oa-module/oa-prevalence-and-burden/
- Psoriasis statistics. (n.d.). https://www.psoriasis.org/psoriasis-statistics/
- Castellanos, J., & Axelrod, D. (1990). Effect of habitual knuckle cracking on hand function. Annals of the Rheumatic Diseases, 49(5), 308–309. https://doi.org/10.1136/ard.49.5.308



